Postpartum
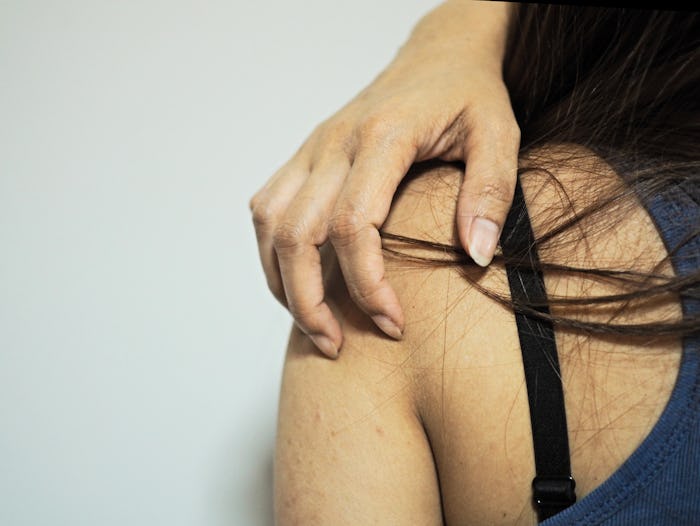
Everything You Need To Know About Postpartum Hives
It won’t last forever.
After finally delivering the baby you’ve carried for more than nine months, you may be surprised when your body continues to produce strange new symptoms related to pregnancy and birth. Postpartum hives are one such condition that can be both puzzling and uncomfortable. Postpartum hives are medically known as pruritic urticarial papules and plaques of pregnancy, or PUPPP. This condition affects about 15% of women either before or after delivery, and can be quite uncomfortable and even painful. The cause is not fully understood, though it's clear that it's an allergic or inflammatory response.
Where do postpartum hives occur?
Postpartum hives can appear anywhere you have skin: face, neck, abdomen, chest, arms, legs, and even down there. They can present as raised bumps that turn white when you press on them, or a red inflamed rash, but more noticeable than the appearance is the sensation. Hives are itchy, sometimes intensely itchy to the point of pain.
Is it normal to get hives after pregnancy?
At Akron Children’s Hospital, Dr. Katherine Wolfe, a maternal-fetal medicine specialist, specializes in high-risk pregnancies and is familiar with the variety of conditions that can plague pregnant women. She tells Romper, “In general, PUPPs is one of the most common dermatoses that occurs during pregnancy.”
When do postpartum hives start?
Typically, if not already present before delivery, they will begin within a few hours to days after delivery. In some rare cases, they can appear up to six weeks after delivery, but the vast majority will occur within the first 48 hours.
How long do postpartum hives last?
Thankfully, PUPPP resolves within days or weeks. “When it happens, it feels like it is never going to end, but commonly this rash will resolve within two weeks after delivery,” says Dr. Betsy Greenleaf DO, a board-certified OB-GYN. She shares her own experience with postpartum hives. “Near the end of my first pregnancy, it began as an itch that I couldn't scratch and turned into a sensation of a severe sunburn.” Postpartum hives can persist for a month to six weeks, but that’s less common, she says.
Are postpartum hives contagious?
Probably not, according to Greenleaf. While there are rare circumstances where postpartum hives could be caused by an infection or virus, odds are that you are not going to spread your hives to your baby or other family members.
What anti-itch medications are safe while breastfeeding?
Wolfe says while hives will resolve in time, there are some treatments that can ease the uncomfortable or painful symptoms. She says you may be prescribed topical systemic corticosteroids (such as a hydrocortisone cream) or over-the-counter oral antihistamines like Claritin and Zyrtec. Prolonged use of antihistamines has been linked to a decreased milk supply for some mothers as well as increased drowsiness. Topical creams should be applied away from any area that has contact with the baby while nursing, and should not be applied to the breast, areola, or nipple area at all.
These potential concerns do not mean that you should stop using the medication. Talk to your doctor about your specific situation. “I worry about the itching causing sleep disruptions,” says Wolfe. “For mothers in the third trimester or newly postpartum, sleep is an important part of her health. I would advise a postpartum breastfeeding mom to have extra help from her partner, family member, friend or doula if she isn’t getting enough sleep and chooses to take an antihistamine. If extra help is not available, I would strongly consider a short course of oral prednisone if conservative measures [like antihistamines and topical treatments] are not working.”
All three of these common treatments — topical creams, oral antihistamines, and oral steroids — have been shown to generally be safe for pregnant and nursing women and their children when used for a short time, says Wolfe.
Holistic postpartum hives treatment
Whether you opt for lotions or antihistamines, there are several non-medical tips for alleviating the itchiness. Greenleaf makes these holistic recommendations:
- Distraction therapy. The itching worsens at night when you have nothing better to focus on than the discomfort. During the day, start a hobby, watch a movie, go for a walk. At night focus on your breath, listen to music, and read a book.
- Ice or cool packs. Apply ice for no more than 20 minutes at a time. Or soak a towel in cool water and place it on the affected area.
- Topical oatmeal. Aveeno makes excellent products with soothing oatmeal that can be used topically to help the itch.
- Avoid hot showers or baths. The heat can dilate blood vessels on the skin, worsening inflammation and rash. Take warm or cool showers and pat your skin dry.
- Try pressing on the area instead of scratching. Scratching can worsen the release of inflammatory chemicals in the skin. In addition, scratching can introduce bacteria into the skin leading to infection.
- Wear loose, soft clothing. Rough fabrics or tight-fitting clothing can trigger more itching.
- Stay well hydrated. Drink enough fluids so that your urine is clear. Hydration helps to moisturize the skin and aids with detoxification. Dry skin can be more brittle and likely to crack.
- Avoid harsh soaps, detergents, and fragrances. In general, pregnant or not, avoiding these chemicals are healthier for the skin but essential if you are experiencing a rash. Aim to use just water or mild cleansers for bathing — wash clothes in dye-free, fragrance-free detergent. Some people swear by pine-tar soap. This is an old-time remedy for rash.
- Avoid inflammatory foods such as sugar, wheat, dairy, and processed foods. These foods can worsen bodily inflammation and irritation.
Can breastfeeding cause postpartum hives?
There does not appear to be any link between breastfeeding and postpartum hives, though the hormonal changes of birth and breastfeeding cause many changes in the body, says Emily Silver, a nurse practitioner and certified lactation consultant.
“However, there has been a reported association from mothers that use of antihistamines, often long term, can lead to them noticing a decrease in their milk supply. This should not stop treatment. If a mother takes an antihistamine and then notices an impact on her supply, she would then let her OB know or a lactation consultant to evaluate risk/benefits for treatment,” says Silver. Hives should not be a deterrent for someone who wants to breastfeed, and also can occur in someone who is bottle feeding.
While an unwelcome complication during late pregnancy and after birth, postpartum hives are not a danger to yourself or you baby and will resolve on their own, especially if you can manage to avoid scratching the itch.
Sources interviewed:
Dr. Betsy Greenleaf, DO, FACOOG, FACOG, OB-GYN and advisor at pH.D Feminine Health
Emily Silver NP-C, IBCLC, international board certified lactation consultant and co-founder of NAPS + Nurture by NAPS
Dr. Katherine Wolfe, DO, FACOG, interim director of maternal-fetal medicine at Akron Children’s Hospital
This article was originally published on